For payers eager to simplify workflows
Enhance member and provider network experiences and compliantly simplify complex payer workflows through intelligent data exchange, machine learning, interoperability, and insights.
and data entry
and patient satisfaction
to care
data entry
and patient satisfaction
Improve Care Delivery, Outcomes and Processes
Unlock Valuable, Actionable Data.
Streamline prior authorizations with our NLP AI-enabled data extraction intelligence to match data, highlights urgent PAs (move to unstructured to structured)
Improve care coordination with real-time health event alert notifications.
Reduce member gaps in care & improve quality measures with real-time event notifications
Scalable, secure, online cloud faxing.
Cut down paper workflow and save operational costs with HITRUST® CSF certified digital cloud-based fax
Why NLP/AI Speeds Prior Authorizations

Streamline the prior authorization workflow by using NLP and AI to reduce the need for human intervention and manual data entry. Consensus Clarity transforms unstructured documents, like electronic faxes and PDFs, to structured intelligent data so important authorization content can be easily consumed into payer systems where prioritization and urgent needs are surfaced for faster approvals.
Why Real-Time Event Notifications Minimizes Gaps

Identify and communicate member utilization data to providers and case managers to improve continuity of care; gaps in care and impact on quality metrics. Alert notifications address critical events including admission, discharge, gaps in care, and lab results that are sent in real-time so you can communicate with your providers.
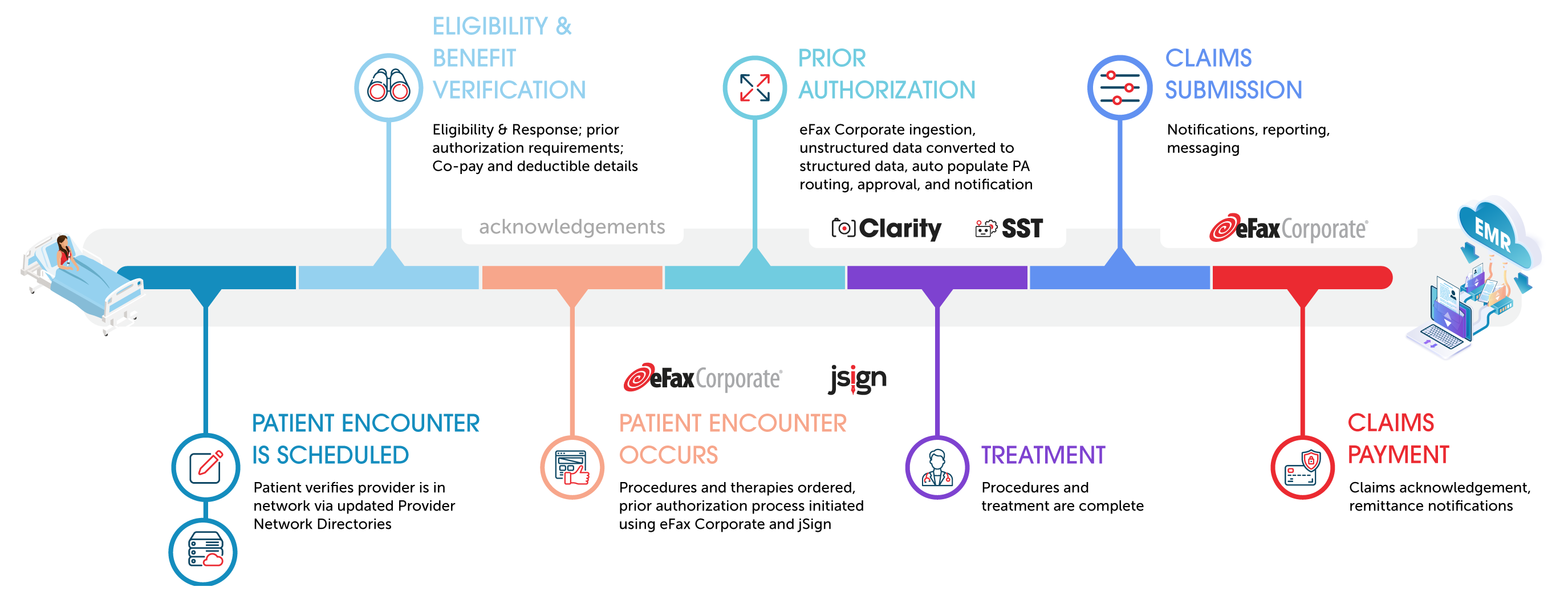
Functionality Map for Payers
Streamline your prior authorization workflow by using NLP and AI and reduce the need for human intervention and manual data entry. By transforming unstructured documents, like electronic faxes and PDFs, to structured intelligent data, important authorization content can be easily consumed into payer systems where prioritization and urgent needs are surfaced for faster approvals.
Zoom